Reference
Berman, A., Snyder, S., Frandsen, G. (2021). Vital Signs. In Kozier & Erb’s Fundamentals of Nursing Concepts, Process and Practice (11th ed., pp. 532-569). Pearson Education
- With additions from Nurse Wong and Nurse Tuiza
Vital signs are traditionally composed of body temperature, pulse, respirations, and blood pressure. In recent times, many agencies have designated pain as a fifth vital sign to be assessed along with the four traditional vital signs (Joint Commission International). This is discussed in this note on Chapter 30 of the book (WIP). Oxygen saturation is also obtained along with the aforementioned, and may be considered the sixth vital sign. Key points:
- Vital signs reflect the functions of the body. Changes in function that are otherwise not observable may be gleaned upon by observing changes in vital signs.
- Vital signs are not routine procedures. Each time vital signs are taken, the nurse must apply their knowledge actively in a thoughtful, scientific assessment that take into consideration the client’s current and previous health status, baseline data, and currently accepted standards for the normal values of vital signs.
- Vital signs are a nurse’s initiative. While vital signs monitoring can be ordered by primary care providers (e.g., urine output q1° post-biopsy of a kidney), this is considered the minimum; a nurse may and should assess more frequently if the client’s health status requires it.
Moments of Vital Sign Taking (mn. ABC)
- Admission for baseline data.
- Before and after any medical or nursing intervention or procedure, especially for those that would affect the vital signs such as digitalis preparations for their negative chronotropic effect.
- Changes in health status such as complaints of pain or an altered level of consciousness.
Delegation of Vital Sign Taking
Assistive Personnel (AP) often take the vital signs in place of the nurse, but they do not bear the responsibility of interpretation of any findings. They must report all findings to the nurse.
The nurse must not delegate non-routine measurements to the AP— medically unstable patients, those who have just undergone from invasive procedures, acute patients, or any patient that the nurse deems as “fragile” cannot be delegated to APs.
Body Temperature
Body temperature is the balance between heat generation and heat loss. In general, there are two types of body heat: core temperature, measured through contact with mucous membranes or directly from organs or muscles, and surface temperature, measured through the skin.
Heat Production
The body’s metabolism is the primary dictator of heat production. The basal metabolic rate itself is the baseline level of metabolism in individuals. Cellular metabolism increases with more muscle activity (exercise, shivering, etc.), higher hormonal function (T₄, epinephrine, and norepinephrine), and other biological functions such as inflammation and fever.
- Age also plays a role in heat production; heat production is generally high in younger ages and gradually decreases as one approaches late adulthood.
Heat Loss
- Radiation: the transfer of heat without direct contact, such as the warmth felt from the sun despite its distance from us.
- Conduction: the transfer of heat through contact.
- Convection: the transfer of heat through contact through drafts and wind— air currents.
- Evaporation: the loss of heat as moisture evaporates from the surface of the body, which carries heat away from the body. This occurs in breathing, exposed mucosa like the mouth, and importantly, sweating.
Multiple factors affect body temperature outside of the body’s biological processes. Variance in body temperature may even be explained through these normal conditions:
- Age: infants and children have greater variances in temperature compared to pubertal children and adolescents/adults. As mentioned earlier, metabolic processes continue to slow into adulthood, with those over 75 years old being at risk for hypothermia and hyperthermia. This occurs as a result of both thermoregulatory and physiologic changes.
- Diurnal Variations: temperature undergoes elevations and depressions in line with an individual’s circadian rhythm. “Diurnal” refers to day time, opposite of “Nocturnal”. The body temperature is normally the lowest from 0400 to 0600 hours and rise by up to 1.0°C at the peak, usually around 1600 and 1800 hours (a 12 hour-cycle).
- Stress: stimulation of the sympathetic nervous system can increase metabolic activity and heat production. Stressed and anxious patients are anticipated to have elevated body temperatures.
- Environment: extremes in environmental temperature can affect a client’s thermoregulatory systems.
Thermoregulation
The hypothalamus (“hypothalamic integrator”) maintains the body’s optimal temperature by working with sensory receptors throughout the body (peripheral and core). These sensors detect cold and warmth and apply physiologic processes accordingly:
- When cold is detected, (a) shivering, rapid contraction and relaxation of skeletal muscles, occurs to produce heat from muscle activity, (b) sweat inhibition to decrease evaporative heat loss, and (c) vasoconstriction to decrease heat loss by distancing the blood from the skin, allowing it to stay “inside”.
- When warmth is detected, the opposite occurs; (a) sweating increases to enhance evaporative cooling, and (b) peripheral vasodilation occurs.
The conscious mind also experiences discomfort with these temperatures and takes steps to thermoregulate, such as through clothing in response to cold or using a fan in response to heat.
Alterations in Body Temperature
Some declarations: normal temperature is considered to be between 36°C and 37.5°C (96.8°F to 99.5°F). Any temperature higher than this is considered pyrexia (“hyperpyrexia” if ≥41°C) and any temperature is considered hypothermia.
- Intermittent Fever: an intermittent fever is one whose temperature alternates between normal temperature and hyperthermia within one day. Common examples of this includes malaria and pulmonary tuberculosis.
- Remittent Fever: a fever that maintains a high temperature with wide fluctuations (>2°C) over 24 hours.
- Relapsing Fever: a fever with short periods (one to two days) of normal body temperature.
- Constant Fever: a fever that maintains a high temperature with small fluctuations in temperature (<2°C) over 24 hours.
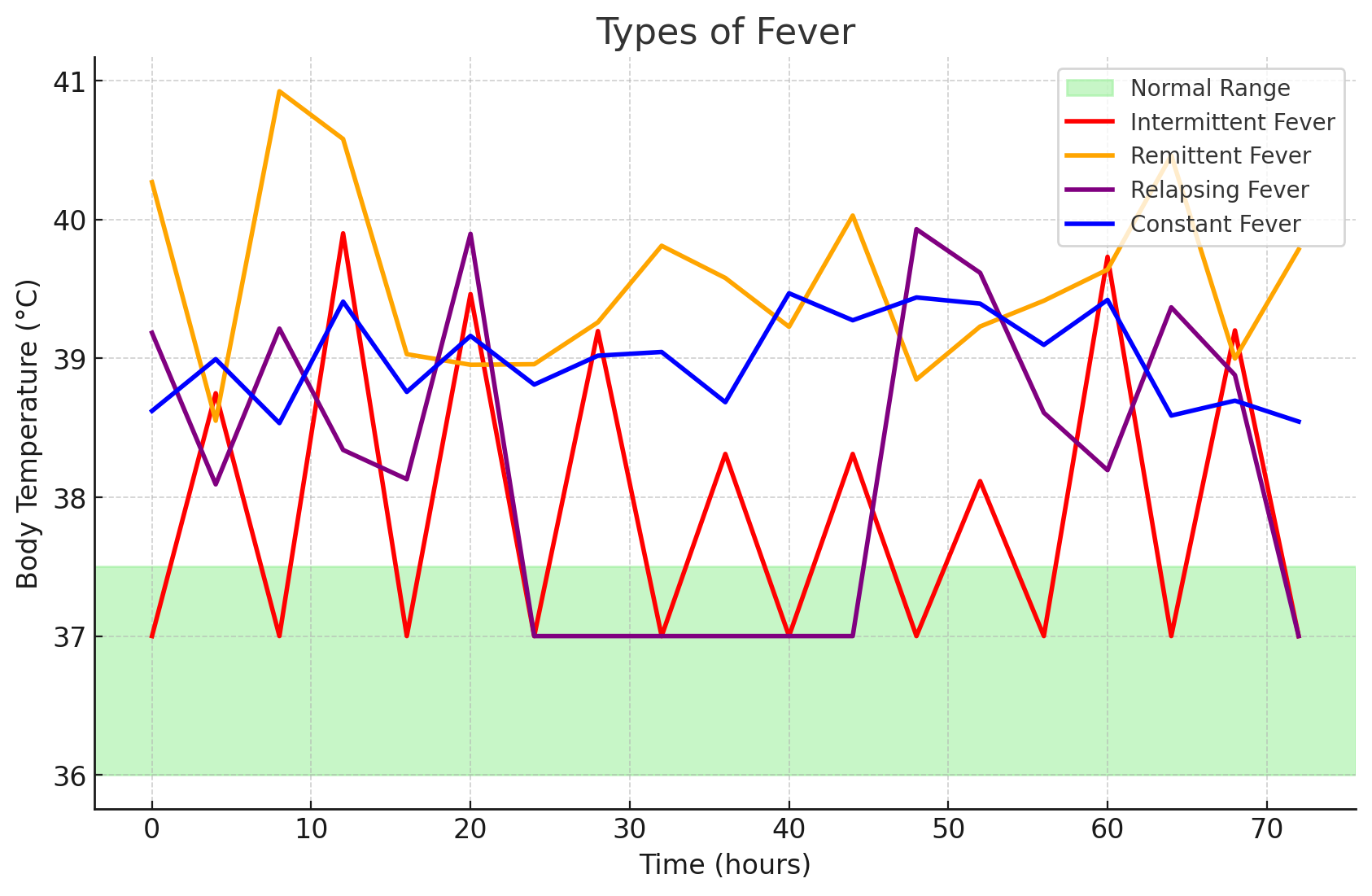
These are simple depictions of the types of fever. Not sourced from the book.
- Fever Spikes: temperatures that rapidly become feverish then returns to normal within a few hours, often due to bacterial blood infections.
- Heat Exhaustion: a source of high temperature that is not a “true” fever caused by biological processes; it is a result of environmental exposure. This is accompanied by paleness, dizziness, nausea, vomiting, fainting, and a moderately increased temperature (38.3°C to 38.9°C [101°F to 102°F]). Higher yet (~41.1°C), the individual stops sweating and the skin feels warm and appears flushed. The individual becomes delirious, potentially becomes unconscious, and may experience seizures. This is a heat stroke.
- Hypothermia: a result of excessive heat loss, inadequate heat production, and impaired hypothalamic thermoregulation. This may be accidental or induced to decrease the oxygen requirement by body tissues such as during certain surgeries. In accidents (exposure to cold environment, immersion in cold water, lack of adequate clothing or heat source), skin and underlying tissues may be damaged by the freezing cold, resulting in frostbite. This commonly occurs in hands, feet, nose, and ears. Patients with hypothermia display decreased body temperature, pulse, respirations, blood pressure, urine output, and level of consciousness progressing down to a coma; severe shivering in early stages; feeling of cold and chills; pale, cool, waxy skin; and lack of muscle coordination.
- Managing hypothermia involves removing the client from the cold and rewarming the client’s body. (a) Mild Hypothermia can be managed with blankets, (b) Severe Hypothermia should be managed with hypothermia blankets and warm IV fluids. A warm environment, dry clothing and head cover, positioning (limbs close to body), warm oral fluids, and warming pads are all methods for rewarming the patient.
Frostbite
- First Degree Frostbite: the skin is intact; it is often only reddened— circulation is intact.
- Second Degree Frostbite: frost has penetrated into the epidermis.
- Third Degree Frostbite: frost has penetrated into the subcutaneous tissue.
- Fourth Degree Frostbite: tissue has become necrotic and blackened.
Assessing Body Temperature
| Site of Measurement | Heat Type and Reference Range | Considerations | Placement |
|---|---|---|---|
| Oral Temperature | Core; 36.5 - 37.5°C | Accessible and convenient. - Patient must be awake and oriented. - This is only used for patients 3 years old and above. - The bulb of the thermometer is placed sublingually, in contact with the side of the frenulum. - Thermometers can break if bitten - Inaccurate if client has just ingested hot or cold food or fluid or smoked. The nurse must wait 30 minutes before taking an oral temperature. - Could injure the mouth following oral surgery. | The tip of the thermometer is placed on either side of the frenulum.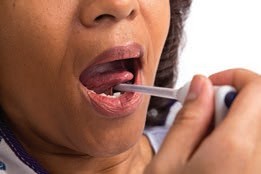 |
| Rectal Temperature | Core; +1°C of oral | Reliable; very accurate. - Clean gloves are used. - Insertion is done during inhalation when the sphincter relaxes. Insertion is 1.5” to 2” for adults and 0.5” to 1” for children. - Inconvenient and more unpleasant for clients; difficult for clients who cannot turn to the side. - Could injure the rectum. Contraindicated for rectal surgery, diarrhea, immunosuppression, and clotting disorders/hemorrhoids. - Presence of stool may interfere with thermometer placement. | Apply clean gloves and instruct the client to take a slow deep breath during insertion. Never force the thermometer if resistance is felt.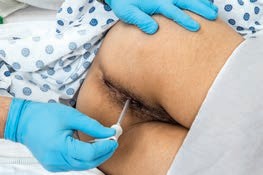 |
| Axillary Temperature | Surface; -1°C of oral; least accurate reading | Safe and noninvasive. Preferred for newborns. This is usually only recommended for adults for whom other temperature sites are contraindicated. - The axilla must be dry (pat dry if damp). Hair may also be a problem. - The thermometer may need to be left in place a long time to obtain an accurate measurement. | Pat the axilla dry if very moist. The tip of the thermometer is placed in the center of the axilla.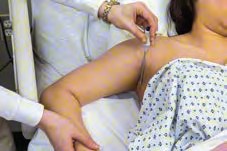 |
| Tympanic Temperature | Core; +0.3°C | Readily accessible; reflects the core temperature; very fast - A fast and accurate method of taking temperature, often used in children. However, it may be uncomfortable, injurious, and affected by cerumen. - Straightening of the ear canal is required for a reading. For children up to three years of age, pull the ear back and down. If older, pull the ear back and up - Can be uncomfortable and involves risk of injuring the membrane if the probe is inserted too far. - Repeated measurements may vary. Right and left measurements can differ if there are anatomic or pathologic differences (e.g., infection). - Presence of cerumen can affect the reading. - Requires proper technique; not too loose nor tight in the use of the probe. | Pull the pinna slightly upward and backward (adult) while inserting the tympanic thermometer. The probe is pointed slightly anteriorly towards the eardrum, and inserted slowly using a rotating motion until snug.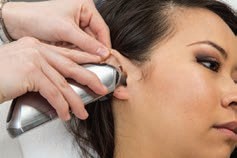 |
| Temporal Temperature | Surface; Same as core temperature. | Safe and noninvasive; very fast. May utilize a patch, chemical thermometer, or temporal artery thermometer. This is useful for infants and children. - Requires electronic equipment that may be expensive or unavailable. Variation in technique needed (forehead-temple) if the client has perspiration on the forehead. | Brush hair aside if covering the temporal artery area. The probe is placed flush midline on the forehead and slowly slid to the hairline, not down the side of the face, then touch it on the neck just behind the earlobe.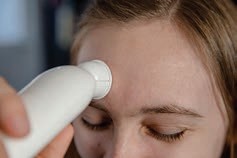 |
Mercury Thermometer Breakage
In the event of the breakage of a mercury thermometer, the nurse requires proper disposal protocol to avoid mercury poisoning. The nurse requires (a) any rubber gloves, (b) paper towels to soak up the mercury, (c) plastic bags for disposal sealed with tape, and (d) a flashlight to scan for beads of mercury. All contaminated materials must be disposed. Disposal via drain and vacuuming and sweeping are dangerous.
Any mercurial thermometers encountered should be promptly recommended for replacement and safe disposal.
Temperature Scales
Kozier utilizes three operations to translate between Celsius and Fahrenheit: (a) a constant subtraction or addition of 32, and (b) multiplication by or .
Personally, I replace or with , and instead change between division and multiplication— °C is smaller than °F, so converting from °F to °C uses subtraction then division; °F is larger than °C, so converting from °C to °F uses multiplication then addition. Whichever is easier to remember for you. 🤷♂️
Temperature Across the Lifespan
- In Infants, temperature is extremely labile due to thermal dysregulation; the hypothalamus is not yet equipped with regulating body temperature.
- The axillary site is preferred; the arm is held against the chest during assessment. The axilla are not as accurate as other routes, but is safe and non-invasive.
- The tympanic route can be used— fast and convenient. The infant is positioned supine and the head is stabilized. The pinna is pulled straight back and slightly downward for children 3 years old and younger, and upward for those older than 3 years old. The probe is directed anteriorly slightly and advanced until the canal is sealed, but not touching the tympanic membrane. This route is avoided with on-going ear infections.
- The rectal route is the least desirable.
- In Children:
- The tympanic or temporal artery sites are preferred. For tympanic route utilization, the same contraindications are in infants is applied. The child is positioned on the adult’s lap and the head is held gently against the adult for support. The pinna is pulled straight back and upward for children over age 3.
- The oral route may be used, but only non-breakable, electronic thermometers are recommended.
- The rectal route places the child prone on the parent’s lap, or side-lying with the knees flexed. The probe is inserted by 1 inch into the rectum.
- In Older Adults:
- Temperatures tend to be lower, and easily affected by environmental and internal temperature changes. They are at risk of both hypothermia and hyperthermia. The inability of the older adult body to generate or maintain heat can cause their temperature to fail as a measure of seriousness of the pathology of a disease (e.g., pneumonia may only manifest a slight temperature elevation). Alternative assessments should also be used.
- Cerumen impaction may occur and affect the tympanic route.
- Hemorrhoids are also more common in older adults; assessment is required prior to the use of rectal thermometers.
Pulse
The pulse is a wave of blood created by contraction of the left ventricle of the heart. Generally, the pulse wave represents the stroke volume output or the amount of blood that enters the arteries with each ventricular contraction. The following are some terms related to pulse:
- Compliance: the ability of arteries to distend (stretch) when pressure is applied by a heart beat, and rebound when the pressure is released.
- Cardiac Output: the amount of blood sent through the body in one minute. This is equal to the stroke volume multiplied by the heart rate. In a resting adult, the heart pumps about 5 liters of blood each minute.
- Stroke Volume: the amount of blood sent through the body with each contraction of the heart.
- Peripheral Pulses: pulses located away from the heart e.g. the foot or wrist.
- Apical (Central) Pulse: the pulse obtained from the apex of the heart, referred to as the point of maximal impulse (PMI)
- Heart Rate: the amount of contractions performed by the heart in one minute.
Factors Affecting the Pulse
- Age: similar to temperature, pulse decreases as age increases.
- Sex: after puberty, the male pulse rate becomes slightly lower than the female pulse rate.
- Exercise: the pulse rate increases with activity depending on cardiac size, strength and efficiency; athletes will experience a slower rate of increase during exercise than the average individual.
- Fever: an elevated body temperature causes vasodilation, which lowers blood pressure, which causes an increased heart rate. A fever also increases metabolic rate, which also contributes to an accelerated pulse.
- Medications: medications that have chronotropic, inotropic, or domotropic effects can increase or decrease pulse rate, strength, and conductivity respectively.
- Hypovolemia or Dehydration: loss of fluid from the vascular system increases the pulse rate as the heart attempts to increase blood pressure.
- Stress: sympathetic nervous stimulation increases the overall activity of the heart in both rate and force. Causes of stress include fear, anxiety, and acute pain.
- Position: dependent positioning (sitting or standing) decreases venous blood return and subsequent reduction in blood pressure, increasing the heart rate.
- Pathology: certain diseases such as heart conditions or those that impair oxygenation can alter the resting pulse rate.
| Age | Pulse Average | Respiration Average |
|---|---|---|
| Newborn | 130 (80-180) | 35 (30-60) |
| 1 year | 120 (80-140) | 30 (20-40) |
| 5-8 years | 100 (75-120) | 20 (15-25) |
| 10 years | 70 (50-90) | 19 (15-25) |
| Teen | 75 (50-90) | 18 (15-20) |
| Adult | 80 (60-100) | 16 (12-20) |
| Older Adult | 70 (60-100) | 16 (15-20) |
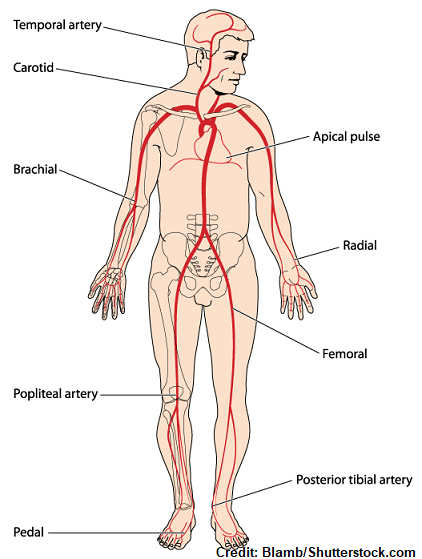
Pulse Sites
- Temporal, where the temporal artery passes over the temporal bone of the head. It is above and to the side (superior and lateral) of the eye.
- Carotid, at the side of the neck where the carotid artery between the trachea and the sternocleidomastoid muscle.
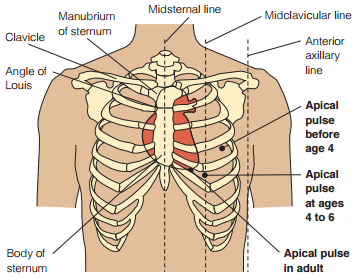
- Apical, at the apex of the heart. In an adult, this is located on the left side of the chest about 8 cm (3 in.) to the left of the sternum (breastbone) at the fifth intercostal space. This may be further left in cardiomegaly. The location of the apical pulse also changes during childhood, illustrated below.
- Brachial, at the inner aspect of the biceps muscle of the arm or medially in the antecubital space.
- Radial, where the radial artery runs along the radial bone, on the thumb side of the inner aspect of the wrist.
- Femoral, where the femoral artery passes alongside the inguinal ligament.
- Popliteal, where the popliteal artery passes behind the knee.
- Posterior tibial, on the medial surface of the ankle where the posterior tibial artery passes behind the medial malleolus.
- Dorsalis pedis, where the dorsalis pedis artery passes over the bones of the foot, on an imaginary line drawn from the middle of the ankle to the space between the big and second toes.
| Pulse Site | Location | Reasons for Use |
|---|---|---|
| Radial | Thumb side, inner aspect of the wrist | Readily accessible |
| Temporal | Temporal bone, supralateral to the eye | Used when radial pulse is not accessible |
| Carotid | Between the trachea and the sternocleidomastoid muscle. | Used during cardiac arrest or shock in adults Used to determine circulation to the brain |
| Apical | 8 centimeters left of the sternum at the fifth intercostal space* | Routinely used for infants and children up to 3 years of age. Used to determine discrepancies with radial nurse Used in conjunction with some medications |
| Brachial | Inner aspect of the biceps muscle; medially in the antecubital space | Used to measure blood pressure Used during cardiac arrest for infants |
| Femoral | Along the inguinal ligament | Used in cases of cardiac arrest or shock Used to determine circulation to a leg |
| Popliteal | Behind the knee | Used to determine circulation to the lower leg |
| Posterior tibial | Medial surface o the ankle behind the medial malleolus | Used to determine circulation to the foot |
| Dorsalis pedis | From the middle of the ankle to the space between the big and second toes | Used to determine circulation to the foot |
Assessing the Pulse
A pulse is commonly asses through palpation or auscultation.
- Palpation: middle three fingers placed on the pulse site; used for all sites except the apex of the heart. The fingers of the hand should apply moderate pressure; too light and a pulse may not be palpated, while too firm and the pulse may be obliterated.
- Auscultation: a stethoscope is used for assessing apical pulses. In difficult-to-assess pulses (usable in noisy environments), a doppler ultrasound stethoscope may be used.
Read and Watch: Nursing Skills: Assessing Peripheral, Apical, and Apical-Radial Pulses
Be Aware
The nurse should be aware of the following:
- Any medication that could affect the heart rate.
- Whether the client has been physically active. If so, wait 10 to 15 minutes until the client has rested and the pulse has slowed to its usual rate.
- Any baseline data about the normal heart rate for the client. For example, a physically fit athlete may have a resting heart rate below 60 beats/min.
- Whether the client should assume a particular position (e.g., sitting). In some clients, the rate changes with the position because of changes in blood flow volume and autonomic nervous system activity.
The pulse can be assessed according to rate, rhythm, volume, arterial wall elasticity, and presence or absence of bilateral equality.
- Rate: >100 beats/min is considered tachycardia and <60 beats/min is considered bradycardia. In either case, if this is observed, the nurse must obtain the apical pulse.
- Rhythm: the pattern and intervals of the beats. In a normal pulse, beats are spaced in equal time intervals. A pulse with an irregular rhythm is referred to as a dysrhythmia or arrhythmia. These appear as random, irregular beats or a predictable pattern of irregular beats (“regularly irregular”). The apical pulse should be assessed if any abnormality is observed, and an ECG is necessary to define the dysrhythmia further.
- Pulse Volume: “strength” or “amplitude”. The force of the blood with each beat, ranging from absent to bounding. Absent pulses are weak and easily obliterated even without moderate pressure, while bounding pulses are strong and difficult to obliterate.
| Grade | Pulse Characteristic |
|---|---|
| 0 | Absent; non-palpable pulses |
| 1 | Weak, thready pulses |
| 2 | Normal; easily distinguishable pulses |
| 3 | Strong pulses; bounding |
- Arterial Wall Elasticity: upon palpation, healthy, normal arteries feel straight, smooth, soft, and pliable. The loss of elasticity often appear as a tortuous (twisted) and irregular artery upon palpation.
- Bilateral Equality: checking for perfusion to a peripheral pulse should also warrant the assessment of the corresponding pulse on the other side of the body. The second assessment gives the nurse data with which to compare the pulses. In assessing perfusion, the nurse starts at the most distal pulse site (e.g., dorsalis pedis) and makes their way up the extremity until a pulse is found.
Patient-Centered Care
Clients can be provided guidance in relation to pulse assessment at home.
- Teach the client to monitor the pulse prior to taking medications that affect the heart rate. The client should know to report any notable changes in heart rate or rhythm.
- Inform the client about activities known to significantly affect pulse rate such as emotional stress, exercise, ingesting caffeine, and sleep. If clients are sensitive to pulse rate changes, they should consider the modification of these activities to stabilize the pulse.
- Lengthy monitoring may use a Holter monitor, an ambulatory recorder usable for 24 hours or longer. Other cardiac event monitors also exist, such as those activated during periods of exacerbation.
Pulse Deficit
A pulse deficit is a difference between apical and peripheral pulses. This warrants an apical-radial pulse assessment.
Pulse Across the Lifespan
- Newborns may have physiologic (expected) heart murmurs. These reflect functional incomplete closure of fetal heart structures (ductus arteriosus or foramen ovale).
- Infants: apical pulse is used up to 2 to 3 years old to establish baseline data, normalcy, and regularity of the rhythm. The infant is placed supine while the infant is comfortable and rested; this necessitates apical pulse assessment ahead of other uncomfortable procedures to avoid artificial elevation of pulse findings.
- Children: the child is placed in the adult’s arms or close to the adult. This may decrease anxiety and yield more accurate results. In apical pulses, children are placed supine or sitting like adults. Prior to assessment, play-based demonstration (with a stuffed animal or doll) may be done along with allowing the child to handle the stethoscope before beginning the procedure. This promotes cooperation and decreases anxiety.
- Older Adults: severe hand or arm tremors may make radial pulse assessment difficult. Peripheral pulses become less reliable in old age due to decreased cardiac output, sclerotic changes, and dysrhythmias. An apical pulse is increasingly more preferred over peripheral pulses. Contrastingly, this weakness of the peripheral pulse warrants assessment of pedal pulses for regularity, volume, and symmetry. This age group also takes a longer period to return to their baseline values after activity.
Respirations
Respiration is the act of breathing. Inhalation or inspiration refers to the intake of air into the lungs. Exhalation or expiration refers to breathing out or the movement of gases from the lungs to the atmosphere. Ventilation is also used to refer to the movement of air into and out of the lungs. There are two types of breathing:
- Costal (thoracic) Breathing: external intercostal muscles and other accessory muscles, such as the sternocleidomastoid muscles. This is observed by the movement of the chest upward and outward.
- Diaphragmatic (abdominal) Breathing: involves the contraction and relaxation of the diaphragm, and it is observed by the movement of the abdomen, which occurs as a result of the diaphragm’s contraction and downward movement.
Respirations are controlled by (a) respiratory centers in the medulla oblongata and the pons of the brain, and (b) chemoreceptors located centrally in the medulla and peripherally in the carotid and aortic bodies. These respond to changes in O2, CO2, and H+ in the arterial blood to adjust respirations accordingly.
Assessing Respirations
Respirations are easily affected by activity and anxiety. Assessment should occur while the patient is resting. However, assessments may be done after exercise specifically to determine the client’s tolerance to activity. Before each assessment, the nurse must be aware of:
- The client’s normal breathing pattern.
- The influence of the client’s health problems on respirations.
- Any medications or therapies that might affect respirations.
- The relationship of the client’s respirations to cardiovascular function.
Respirations may be characterized by rate, depth, rhythm, quality, effectiveness, ease, and adventitious sounds.
- Rate: normally described in breaths per minute. Fast breathing is termed tachypnea, slow breathing is termed bradypnea, and normal breathing in rate and depth is eupnea. Refer to the table under Pulse for age-based ranges of respiratory rates. Apnea is a cessation of breathing for any period of time.
Sleeping Respirations
A sleeping adult can have respirations lower than 10 breaths/min. Other vital signs must be used to validate the client’s condition.
- Volume: the amount of air (in liters) moving through the lungs. Hyperventilation results in an overexpansion of the lungs characterized by rapid and deep breaths, and hypoventilation results in an underexpansion of the lungs characterized by shallow respirations.
- Rhythm: many alterations of rhythm exist, but two common altered breathing patterns and sounds are Biot breathing (several short breaths followed by long, irregular periods of apnea) and Cheyne-Stokes breathing (waxing and waning, then temporary apnea).
- Ease or Effort: dyspnea is a general term for difficult and labored breathing during which the individual has a persistent, unsatisfied need for air and feels distressed. Orthopnea is dyspnea that occurs when in supine positions, and relieved by sitting upright, standing, or with the orthopneic position.
- Breath Sounds: sounds produced as air travels through the lungs and airways.
- Secretions: the expectoration of various substances from the respiratory tract such as blood (hemoptysis), sputum (productive cough), or the absence of any substance (nonproductive cough).
- Effectiveness: a measurement of whether or not the respirations are adequately oxygenating the blood and excreting carbon dioxide. This is quantified through oxygen saturation measurements via Oximetry
Factors Affecting Respirations
- Rate: exercise, stress, and environmental factors (temperature, altitude [oxygen]), and some medicines can increase metabolism and sympathetic nervous system stimulation.
- Depth: normal inspiration and expiration takes in about 500 mL of air— the tidal volume. This may become deep or shallow with the same factors that affect rate, and positioning. Positions that allow better expansion of the chest will allow for a greater depth and tidal volume. A common complication related to this is supine leading to poor lung aeration, predisposing patients to the stasis of fluids and subsequent infection. Hyperventilation refers to very deep and rapid respirations; hypoventilation refers to very shallow respirations.
- Rhythm refers to the regularity of the expirations and inspirations. These are normally evenly spaced, but can become irregular. Abnormal respiratory rhythms are further discussed in Chapter 49: Oxygenation
- Quality or Character: aspects of breathing that are different from normal, effortless breathing. Two common aspects to consider is the amount of effort required (e.g., labored breathing) and breath sounds (e.g., wheezes).
- Sound of Breathing: normal breathing is silent, but a number of abnormal sounds such as a wheeze are obvious to the nurse’s ear. Many sounds occur as a result of the presence of fluid in the lungs and are most clearly heard with a stethoscope. The following are breath sounds that are audible without amplification:
- Stridor: a shrill, harsh inspiratory sound due to laryngeal obstruction.
- Stertor: snoring or sonorous respiration, usually due to a partial obstruction of the upper airway.
- Wheeze: a continuous, high-pitched “musical” squeak or whistling expiratory sound.
- Bubbles: gurgling sounds heard as air passes through moist secretions in the respiratory tract.
Changes in Respirations Across the Lifespan
- Infants and Children: crying and anxiety will alter the respiratory rate.
- Infants and Young Children may breathe diaphragmatically. In rapid breathing, the nurse may place a hand on the abdomen to feel the rapid rise and fall during respirations.
- Most newborns are complete nose breathers, so nasal obstruction can be life-threatening. They can also experience “periodic breathing” where a pause for a few seconds occur between respirations which may be normal, but parents should be alert to prolonged or frequent pauses (apnea) that require medical attention.
- Older adults experience anatomic and physiologic changes that cause the respiratory system to be less efficient. Any changes in rate or type of breathing should be reported immediately.
| Breathing Pattern | Description |
|---|---|
| Costal/Thoracic Breathing | Breathing facilitated by the thoracic muscles/costals. Breathing in this way expands the thorax. |
| Diaphragmatic/Abdominal Breathing | Breathing facilitated by the diaphragm, the major respiratory muscle of the body. Breathing in this way expands the abdomen. |
| Eupnea | Normal breathing pattern |
| Tachypnea | Increased rate of breathing |
| Bradypnea | Decreased rate of breathing |
| Apnea | The cessation of breathing |
| Cheyne-Stokes Respirations | Rapid, shallow breathing interrupted by periods of apnea. |
| Kussmaul Respirations/Hyperventilation | Rapid, deep breathing often found in acidosis. |
| Biot Respirations | Irregular; non-rhythmic breathing patterns. This may be observed when the medulla oblongata has been damaged. |
| Apneustic | Prolonged inhalation and shortened exhalation breathing. |
| Agonal Breathing | Failure to breath due to brainstem injury |
Blood Pressure
Arterial blood pressure is the pressure placed on the blood vessels by the heart during its systolic (contractile) and diastolic (relaxed) phases.
- Systolic Pressure: the blood pressure at the moment of ejection/during contraction of the heart.
- Diastolic Pressure: the blood pressure at the moment of filling/relaxation of the heart.
- Pulse Pressure: the pressure difference between systolic and diastolic () that indicates the amount of pressure produced by a contraction of the heart, which is often used to reflect fluid status of an individual. It normally sits around 40 mm Hg and ranges from 30 to 50 mm Hg. A consistently heightened pulse pressure occurs in arteriosclerosis, and a low pulse pressure occurs in conditions such as severe heart failure.
- Mean Arterial Pressure: the actual pressure actually delivered to the body’s organs. There are a few ways to calculate this value. Try to check which one is the easiest to remember or to perform.
- (1) Calculating MAP:
- (2) Calculating MAP:
- (3) Calculating MAP:
Normal Blood Pressure Ranges
The American Heart Association (AHA) applies classifications of hypertension with the following criteria:
Category Systolic Blood Pressure Diastolic Blood Pressure Normal <120 mm Hg and <80 mm Hg Elevated (Prehypertension) 120-129 mm Hg and <80 mm Hg Hypertension I 130-139 mm Hg or 80-89 mm Hg Hypertension II 140+ mm Hg or 90+ mm Hg Hypertensive Crisis 180+ mm Hg and/or 120+ mm Hg
Determinants and Factors Affecting Blood Pressure
Determinants are the aspects that make up the pressure forces measured in blood pressure.
- Pumping Action of the Heart: weaker pumping equates to lower cardiac output, and decreased blood pressure. The opposite is also true.
- Peripheral Vascular Resistance: vascular capacity (internal diameter of capillaries and arterioles), arterial compliance, and blood viscosity affect peripheral vascular resistance— the pressure the blood has to fight against to flow. Increased vasoconstriction (such as in smoking), increased viscosity, or arteriosclerosis are all causes for increasing peripheral vascular resistance, increasing blood pressure.
- Blood Volume: blood volume is proportional to blood pressure. In cases of fluid overload from rapid IV infusion or pregnancy, blood pressure increases.
- Blood Viscosity: thick blood (hemoconcentration; Hct > 60%-65%) makes blood more resistant to flow, necessitating an increased blood pressure.
Factors are extraneous conditions that contribute to blood pressure, but is not directly a constituent of blood pressure.
- Age: newborns have a systolic pressure of about 75 mm Hg, which rises with age, reaching its peak during puberty, then declines somewhat. In older adults, arteriosclerosis elevates systolic and even diastolic pressure.
- Exercise: physical activity increases cardiac output and hence blood pressure. For reliable assessment of resting blood pressure, wait 20 to 30 minutes following exercise.
- Stress: stimulation of the sympathetic nervous system increases cardiac output and vasoconstriction of the arterioles, thus increasing the blood pressure reading; however, severe pain can decrease blood pressure greatly by inhibiting the vasomotor center and producing vasodilation.
- Race: African American individuals older than 35 years tend to have higher blood pressures than other races of the same age.
- Sex: females usually have lower blood pressures than males of the same age after puberty, raising after menopause. This difference is thought to be due to hormonal variations. After the age of 65, the rate of high blood pressure is higher in women than it is in men of the same age.
- Medications: caffeine and many other medications may increase or decrease the blood pressure.
- Obesity: childhood and adult obesity is a major predisposing factor for hypertension.
- Diurnal Variations: similar to temperature, blood pressure is the lowest in early morning and peaks in the late afternoon or early evening.
- Medical Conditions: any condition affecting cardiac output, blood volume, blood viscosity, or compliance of the arteries has a direct effect on the blood pressure.
- Temperature: increased temperature from a fever increases metabolic rate, which increases blood pressure. However, in external heat vasodilation occurs which decreases blood pressure. Inversely, cold will cause vasoconstriction and increase blood pressure.
Alterations in Blood Pressure
Hypertension is a persistent elevation of blood pressure. A single elevated blood pressure reading indicates the need for reassessment— a diagnosis is only made after two elevated measurements measured at different times. In most cases, hypertension is asymptomatic and is often a contributing factor to myocardial infarctions (heart attacks).
- Primary Hypertension: the most common form of hypertension, whose cause is unknown.
- Secondary Hypertension: hypertension resultant of known causes.
Factors associated with hypertension include thickening of the arterial walls, which reduces the size of the arterial lumen, and inelasticity of the arteries, as well as lifestyle factors as cigarette smoking, obesity, heavy alcohol consumption, lack of physical exercise, high blood cholesterol levels, and continued exposure to stress.
Hypotension is a blood pressure that is below normal, that is, a systolic reading consistently between 85 and 110 mmHg in an adult whose normal pressure is higher than this. Orthostatic Hypotension (postural hypotension) is a blood pressure that decreases when the client changes from a supine to a sitting or standing position, often the result of peripheral vasodilation in which the blood leaves the central body organs, especially the brain, and moves to the periphery, often causing the client to feel faint.
Assessing for Orthostatic Hypotension
- Place the client in a supine position for at least five minutes, then record the client’s pulse and blood pressure.
- Assist the client to a seated or standing position. Immediately recheck the pulse and blood pressure in the same sites as previously, then again in three minutes.
- Record the results. A drop in blood pressure of 20 mmHg systolic or 10 mmHg diastolic or an increase of 20 beats/min indicates orthostatic hypotension.
Hypotension may be caused by analgesics such as meperidine hydrochloride (Demerol), bleeding, severe burns, and dehydration. It is important to monitor hypotensive clients carefully to prevent falls.
Assessing Blood Pressure
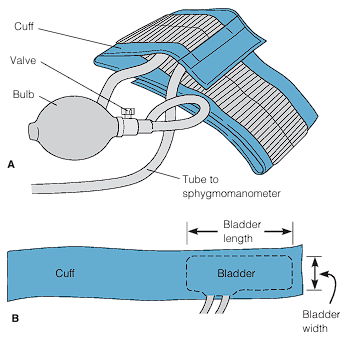
Manual blood pressure management is performed with a blood pressure cuff, a sphygmomanometer, and a stethoscope. The cuff consists of a bag (bladder) that is inflated with air. To the bladder, there are two tubes that connect the pump (bulb) and the sphygmomanometer, which displays the pressure in the bag. There are two types of sphygmomanometers: aneroid, which is a gauge with a calibrated dial with a needle that points to the calibrations; and digital, which eliminates the need to auscultate the client’s systolic and diastolic blood pressures through a stethoscope. Doppler ultrasound stethoscopes are also used to assess blood pressure, especially useful for infants, obese clients, and clients in shock where blood pressure sounds are difficult to hear.
Choosing Blood Pressure Cuff Sizes
- Bladder Width: 40% of the arm circumference, or 20% wider than the diameter. Erroneously high readings are found if the width is too narrow, and vice versa.
- Bladder Length: at least two-thirds of the limb’s circumference.
The most common site for blood pressure assessment is the upper arm, but it may be measured from the forearm, wrist, or thigh in case of contraindications. These contraindications include:
- The site for assessment is injured or diseased.
- The limb for assessment has a cast or bulky bandage.
- The client has had surgical removal of breast or axillary (or inguinal) lymph nodes on that side.
- The client has an IV infusion or blood transfusion in that limb.
- The client has an arteriovenous fistula (e.g., for renal dialysis) in that limb.
Blood pressure may be measured directly or indirectly. Direct (invasive) monitoring involves the insertion of a catheter into the brachial, radial, or femoral artery. Arterial pressure is represented as wavelike forms displayed on a monitor. With correct placement, this pressure reading provides very highly accuracy. As nurses, most measurements will be done noninvasively; indirectly. This may be done with two techniques:
- Auscultatory Method: the use of a stethoscope to listen for Korotkoff sounds, particularly phase 1 and phase 5, to determine the systolic and diastolic blood pressures respectively.
- Korotkoff Phase 1: “A sharp tapping”, which gradually becomes more intense.
- Korotkoff Phase 2: “A swishing or whooshing sound”.
- Korotkoff Phase 3: “A thump softer than the tapping in phase 1”, which sounds crisper and more intense but again softer than in phase 1.
- Korotkoff Phase 4: “A softer blowing muffled sound that fades”. In some institutions, this may be considered the “first diastolic measurement”.
- Korotkoff Phase 5: “Silence”. The pressure level when the last sound is heard. This is the diastolic pressure commonly recorded.
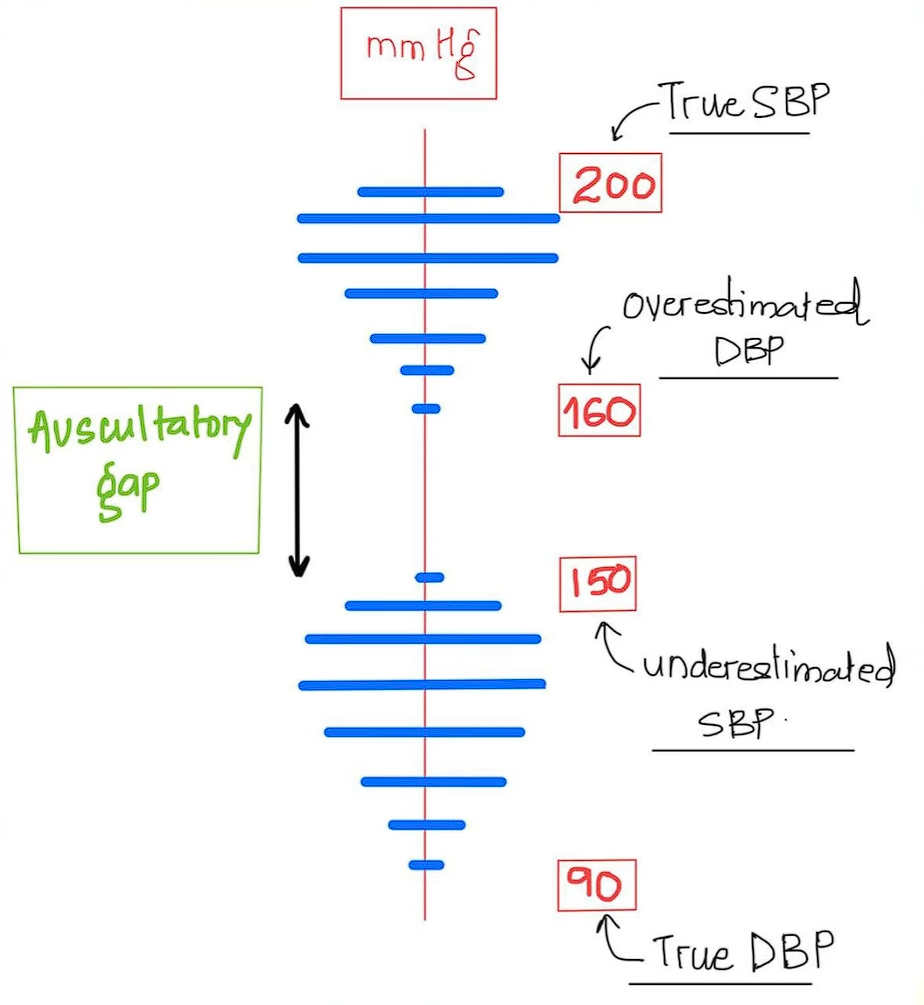
Auscultatory Gap
The auscultatory gap is a phenomenon where phase 1 to phase 3 of the Korotkoff sounds become difficult to hear and appear as silence, even when the pulse is still palpable. This results in an underestimated systolic blood pressure and an overestimated diastolic blood pressure. This phenomenon is demonstrated and explained by Dr. Sourya Acharya (also the source of the following image).
- Palpatory Method: this method is less common, but is used when Korotkoff sounds cannot be heard and electronic equipment to amplify the sounds is not available, or to prevent misdirection from the presence of an auscultatory gap. Similar to the auscultatory method, the nurse uses light to moderate pressure to palpate the pulsations of the artery as the pressure in the cuff is released. The first pulsation felt after releasing the pressure in the cuff is the systolic pressure. A single whiplike vibration, felt in addition to the pulsations, identifies the point at which the pressure in the cuff nears the diastolic pressure. This vibration is no longer felt below the diastolic pressure.
Preparation
Patients must rest approximately 15 minutes after activity for an accurate blood pressure reading. For those who are caffeinated or have smoked, a 30 minute rest period is given in order to obtain an accurate reading. When reading, the patient is seated if possible.
The nurse inflates the cuff one to two inches above the brachial artery (if being taken at the popliteal fossa) up to 30 to 50 mm Hg above the pressure where the pulse becomes obliterated. Once deflated slowly (2 to 3 mm Hg/s), there are five Korotkoff sounds that the nurse hears:
- Korotkoff 1: the first tap or thud indicating the return of blood flow, representing the systolic pressure.
- Korotkoff 2: a swishing or whooshing
- Korotkoff 3: a thumping sound
- Korotkoff 4: a blowing sound
- Korotkoff 5: The following silence. The point at which the diastolic has returned, and is recorded as the diastolic pressure.
Mistakes in Blood Pressure Taking
Error Effect Bladder cuff too narrow Erroneously high Bladder cuff too wide Erroneously low Arm unsupported Erroneously high Insufficient rest before the assessment Erroneously high Repeating assessment too quickly Erroneously high systolic or low diastolic readings Cuff wrapped too loosely or unevenly Erroneously high Deflating cuff too quickly Erroneously low systolic and high diastolic readings Deflating cuff too slowly Erroneously high diastolic readings Failure to use the same arm consistently Inconsistent measurements Arm above level of the heart Erroneously low Assessing immediately after a meal or while client smokes or has pain Erroneously high Failure to identify auscultatory gap Erroneously low systolic pressure and erroneously low diastolic pressure
Read the following for a comprehensive discussion on the skill of Assessing Blood Pressure
Blood Pressure Across the Lifespan
- Infants:
- A pediatric stethoscope should be used.
- The lower edge of the blood pressure cuff can be closer to the antecubital space of an infant.
- Use the palpation method if auscultation is unsuccessful.
- Arm and thigh pressures are equivalent in children under 1 year of age. (There is a difference of 20 to 30 mmHg in the systolic pressures of the arm and thigh in adults)
- The systolic blood pressure of a newborn averages about 70 mmHg, but is not usually recorded due to technical difficulty except when problems are suspected.
- Children:
- Blood pressure should be measured in all children over 3 years of age and in children less than 3 years of age with certain medical conditions.
- All steps of the procedures and what it will feel like should be explained. A demonstration on a doll can be done.
- Use the palpation technique for children under 3 years old.
- Cuff bladder width should be 40% and length should be 80% to 100% of the arm circumference.
- Diastolic pressure is considered to be based on Korotkoff sounds phase 4 rather than phase 5 in children.
- Arm and thigh pressures differ by about 10 mmHg.
- In children, normal blood pressure can be determined quickly with the formula .
- Older Adults:
- Skin may become fragile. Cuff pressure should not be kept high for any longer than necessary.
- Clients may be taking antihypertensives. Determine when the last dose was taken, if any.
- Medications that cause vasodilation and also the loss of baroreceptor efficiency in older adults place them at an increased risk for having orthostatic hypotension. Assess for orthostatic hypotension.
- If the client has arm contractures, assess the blood pressure by palpation, with the arm in a relaxed position. A wrist or thigh reading may be taken if this is not possible.
Oxygen Saturation
A pulse oximeter is a noninvasive device that estimates a client’s blood oxygen saturation (SpO₂) by means of a sensor attached to the client’s finger, toe, nose, earlobe, or forehead (or around the hand or foot of a neonate). The oxygen saturation value is the percent of all hemoglobin binding sites that are occupied by oxygen. The pulse oximeter can detect hypoxemia (low oxygen saturation) before clinical signs and symptoms develop.
Normal oxygen saturation is 95% to 100%; below 90% should be evaluated and treated, and below 70% is life-threatening.
The following are some constraints or factors that affect the viability of an oxygen saturation reading.
- Hemoglobin: saturation is not related to the amount of red blood cells actually present. A patient with low hemoglobin can still obtain a normal reading of 100% SpO₂ despite compromised oxygen capacity.
- Circulation: oximeters rely on circulation to an area to obtain readings. An area with impaired circulation is not a viable site for pulse oximetry. This includes transient causes such as vasoconstriction from cold temperatures or long-standing disease processes such as peripheral vascular diseases.
- Activity: shivering or excessive movements of the sensor site may interfere with accurate readings.
- Light Interference: sensors often use light as the medium of measurement. Readings may be altered by exposure to light such as sunlight or a bilirubin light.
- Carbon monoxide poisoning: pulse oximeters cannot tell the difference between hemoglobin bound with oxygen and hemoglobin bound with carbon monoxide.
Pulse Oximetry Across the Lifespan
- Infants: an earlobe or forehead sensor may be required if fingers, feet, and toes are not available.
- Children: anxiety may be present. Inform the child that the sensor will not hurt. The probe may be disconnected whenever possible to allow for movement of the child.
- Older Adults: vasoconstrictive medications, poor circulation, or thickened nails may interfere with readings. A forehead or earlobe sensory may be used if indicated.
Salient Points
The six vital signs, body temperature, pulse, respirations, blood pressure, pain, and oxygen saturation are measures of an individual’s functioning and health status. Obtaining vital signs are a thoughtful, scientific assessment that takes the client’s current and previous health status, baseline data, and standards into consideration for evaluation of the client’s health.
- Moments of Vital Signs Taking: admission, before and after intervention, and changes in health status
- Delegation: vital signs taking may be delegated if the client is in stable condition; however, the interpretation of the results is not delegated.
Body Temperature:
- Body temperature is the sum value of heat production (metabolism, activity hormones) and heat loss (radiation, conduction, convection, evaporation) over time.
- Body temperature naturally fluctuates throughout the day (diurnal variation), and is affected by age, stress, and the environment (external temperature).
- The thermoregulatory center of the body is the hypothalamus, which reacts to cold by shivering, inhibiting sweat and vasoconstriction; and to heat by sweating and vasodilation.
- The normal body temperature is 36°C to 37.5°C. Hypothermia is <36°C, pyrexia is >37.5°C, and hyperpyrexia is ≥41°C.
- Fevers may take four forms: intermittent, remittent, relapsing, and constant.
- Heat-related conditions such as heat exhaustion and heat stroke can occur with extreme exposure to environmental heat.
- Hypothermia can be mild (managed with blankets) or severe (managed with a hypothermia blanket and warm IV fluids). A warm environment, dry clothing, head cover, positioning, warm oral fluids, and warming pads may be used.
- ,
| Site of Measurement | Considerations | Placement |
|---|---|---|
| Oral Temperature | Accessible and convenient. - Patient must be awake and oriented. - This is only used for patients 3 years old and above. Children may bite and break the thermometer. | The tip of the thermometer is placed on either side of the frenulum. |
| Rectal Temperature | Reliable; very accurate. - Presence of stool may interfere with thermometer placement. - Least desirable site for infants. | Apply clean gloves and instruct the client to take a slow deep breath during insertion. Never force the thermometer if resistance is felt. |
| Axillary Temperature | Safe and noninvasive. Preferred for newborns. This is usually only recommended for adults for whom other temperature sites are contraindicated. - The thermometer may need to be left in place a long time to obtain an accurate measurement. | Pat the axilla dry if very moist. The tip of the thermometer is placed in the center of the axilla. |
| Tympanic Temperature | Readily accessible; reflects the core temperature; very fast - A fast and accurate method of taking temperature, often used in children. However, it may be uncomfortable, injurious, and affected by cerumen. - Presence of cerumen can affect the reading. | For children up to three years of age, pull the ear back and down. If older, pull the ear back and up. The probe is pointed slightly anteriorly towards the eardrum, and inserted slowly using a rotating motion until snug. |
| Temporal Temperature | Safe and noninvasive; very fast. This is useful for infants and children. - Requires electronic equipment that may be expensive or unavailable. Variation in technique needed (forehead-temple) if the client has perspiration on the forehead. | Brush hair aside if covering the temporal artery area. The probe is placed flush midline on the forehead and slowly slid to the hairline, not down the side of the face, then touch it on the neck just behind the earlobe. |
Pulse:
- A pulse is a wave of blood created by contraction of the left ventricle of the heart, representing the stroke volume output.
- A normal pulse rate is 60 to 100 in adults. This is high in newborns (80-180) and trends downwards to adulthood.
- Age, sex, exercise, fever, medications, hypovolemia, stress, positioning, and various pathologies can alter pulses.
- The nine pulse sites are the temporal, carotid, apical, brachial, radial, femoral, popliteal, posterior tibial, and dorsalis pedis pulses. Peripheral pulses may be obtained to determine adequate perfusion to an extremity or the brain (carotid). The most representative pulse site is the apical pulse.
- Pulse assessment may be palpatory (middle three fingers applying moderate pressure on a peripheral pulse site) or auscultatory (apical pulse). A DUS may also be used to amplify pulse sounds.
- A heart rhythm refers to the pattern of heart sounds. Regularity is an important aspect of a healthy heartbeat.
- A pulse deficit is a difference between palpated radial pulses and auscultated apical pulses. The radial-apical technique may be used to check.
- Newborns have physiologic, expected murmurs.
- Roleplay may be a useful tool to reduce anxiety in children.
| Grade | Descriptors |
|---|---|
| 0 | Absent; non-palpable pulses |
| 1 | Weak, thready pulses |
| 2 | Normal; easily distinguishable pulses |
| 3 | Strong pulses; bounding |
Respirations:
- Breathing is regulated by the medulla oblongata and the pons of the brain; and chemoreceptors located centrally in the medulla and peripherally in the carotid and aortic bodies. This normally sits at a rhythm of 12 to 20 breaths/min in an adult.
- Breaths are characterized based on rate, depth, rhythm, quality, effectiveness, ease, and sounds— bradypnea, tachypnea, apnea, hyperventilation, hypoventilation, Biot breathing, Cheyne-Stokes breathing, dyspnea, orthopnea, hemoptysis, productive cough, nonproductive cough, ineffective breathing, stridor, stertor, wheeze, bubbles.
Blood Pressure:
- Arterial blood pressure is the pressure placed on the blood vessel by the heart during its systolic and diastolic phases.
- Normal blood pressure is <120 mm Hg and <80 mm Hg.
- Determinants of Blood Pressure: pumping action of the heart, peripheral vascular resistance, blood volume, blood viscosity.
- Factors of Blood Pressure: age, exercise, stress, race, sex, medications, obesity, diurnal variations, medical conditions, and temperature.
- Hypertension may be primary or secondary.
- Hypotension may be orthostatic. Assess accordingly.
- Observe for the auscultatory gap
- Auscultation of the Korotkoff sounds: P₁ (sharp, tapping), P₂ (swishing), P₃ (thumping), P₄ (soft, muffled), P₅ (silence).
- Cuff size is imperative for accurate readings: 40% width, 2/3rds circumference
Pulse Oximetry:
- Pulse oximetry is an estimation of blood oxygen saturation. This is normally 95% to 100%.
- Avoid errors in pulse oximetry by eliminating motion and light interference.
- Avoid client injury by changing sites for spring-tension type sensors every 2 hours and adhesive type sensors every 4 hours and inspecting the skin.
| Vital Sign | Normal Value | Wait Period |
|---|---|---|
| Body Temperature | 36°C–37.5°C | 30 minutes |
| Pulse | 60–100 | 15 minutes |
| Respirations | 12–20 | a few minutes |
| Blood Pressure | <120/<80 | 30 minutes |
| Pulse Oximetry | 95%–100% |