Cystic Fibrosis
Cystic fibrosis (CF) is a condition characterized by exocrine (mucus-producing) gland dysfunction that produces multisystem involvement. Abnormal transport of sodium and chloride across epithelium leads to increased viscosity of airway mucus, abnormal mucociliary clearance, and lung disease.
The dysfunction of ion transport result in CF, which is characterized by thick, viscous secretions in the lungs, pancreas, liver, intestine, and reproductive tract as well as increased salt content in sweat gland secretions. The primary factor responsible for many clinical manifestations of the disease is mechanical obstruction caused by the increased viscosity of mucous gland secretions. Small passages in organs such as the pancreas and bronchioles become obstructed as secretions precipitate or coagulate to form concretions in glands and ducts.
flowchart LR
B(Abnormal mucus secretion<br>and obstruction)
C1(Bronchi)
C2(Small<br>intestine)
C3(Pancreatic<br>ducts)
C4(Bile<br>ducts)
C5(Obstructed Gamete<br>Passageways)
C1a(Chronic<br>bronchial<br>pneumonia)
C1b(Generalized<br>obstructive<br>emphysema)
C2a(Intestinal obstruction<br>of newborn)
C3a(Malabsorption<br>syndrome)
C4a(Portal<br>hypertension)
C5a(Subfertility)
B-->C1
B-->C2
B-->C3
B-->C4
B-->C5
C1--Bronchial<br>obstruction-->C1a
C1--Bronchial<br>obstruction-->C1b
C2--Inspissated<br>meconium-->C2a
C3--Pancreatic<br>achylia-->C3a
C4--Biliary<br>cirrhosis-->C4a
C5-->C5a
Clinical Manifestations
- Respiratory System: chronic bronchial pneumonia occurs. Often, this is an indicator for the presence of cystic fibrosis when the child has a history of six or more hospitalizations due to pneumonia in a year.
- Chronic coughing, which may be productive or nonproductive.
- Diffuse bronchial and bronchiolar obstruction becomes a chronic obstructive pulmonary disorder; emphysema and bronchiectasis may appear.
- Because of air trapping, a barrel chest appearance can be observed.
- Clubbing and cyanosis can occur with significant gas exchange impairment.
- Gastrointestinal Tract:
- Obstruction of the common pancreatic ducts at the duodenum by thick secretions prevents the release of pancreatic enzymes trypsin, lipase, and amylase. This creates malabsorption as these enzymes are necessary for digestion, especially for fats.
- Fats are necessary to carry fat-soluble vitamins (A, D, E, K) into the body. Avitaminosis can occur without proper fat digestion and absorption.
- Stool bulk increases with undigested proteins and fats, also resulting in the presence of fat in the stool— steatorrhea.
- Malabsorption will result in growth failure and weight loss. Anorexia may also occur due to difficulty of breathing and chronic coughing.
- Obstruction of the common pancreatic ducts at the duodenum by thick secretions prevents the release of pancreatic enzymes trypsin, lipase, and amylase. This creates malabsorption as these enzymes are necessary for digestion, especially for fats.
- Reproductive System:
- Subfertility may appear due to mucous obstruction of the vas deferens, the fallopian tubes, or even the ovaries.
Diagnostic Evaluation
- Sweat Chloride Test: the defect fails to re-absorb chlorine and sodium back into the body from the sweat glands. This results in a characteristic finding of high levels (by as high as four to six times) of chloride and sodium electrolytes in the sweat.
- Normal Levels: 40–60 mEq/L
- Chest Radiography shows patchy atelectasis and obstructive emphysema.
- Newborn Screening and DNA Testing can show the known defective mutations.
Management
- Airway Clearance Therapy (ACTs): Postural Drainage, CPT, Mucolytics/Expectorants, Bronchodilators
- Treatment of Colonization/Pneumonia: antibiotics based on sputum cultures, prevention of contamination (e.g., avoid crowded areas, avoid persons with infections)
- Pancreatic Supplementation: replace pancreatic enzymes with oral supplements taken before meals. Multivitamins (especially the fat-soluble vitamins) are also given as compensation.
- Diet is high-calorie, high-protein, with unrestricted fats.
- Infertility Treatments:
- Gamete Intrafallopian Transfer (GIFT): placement of sperm and eggs into the fallopian tube.
- Zygote Intrafallopian Transfer (ZIFT): placement of an already-fertilized zygote into the fallopian tube.
- Artificial Insemination (AI)
- By Source: the (a) husband, or a (b) donor
- By Placement: the (a) cervical canal, or the (b) uterine cavity
- In-vitro Fertilization (IVF): the method used for patients whose fallopian tubes are non-viable, such as in CF. Compared to ZIFT, the IVF zygote stays in extrauterine conditions for longer and will be placed directly into the uterus.
Pyloric Stenosis
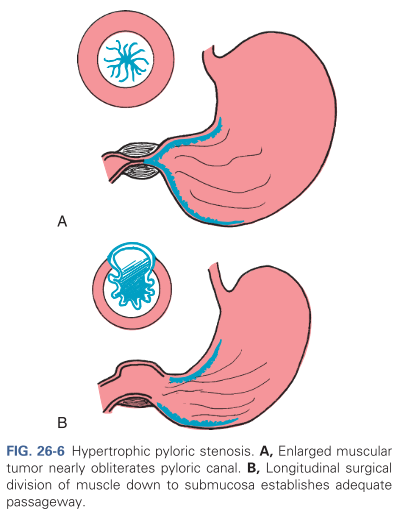
Hypertrophic pyloric stenosis (HPS) occurs when the circumferential muscle of the pyloric sphincter becomes thickened, resulting in elongation and narrowing of the pyloric canal. This produces an outlet obstruction and compensatory dilation, hypertrophy, and hyperperistalsis of the stomach. This condition usually develops in the first few weeks of life, causing nonbilous vomiting, which occurs after feeding; projectile vomiting may develop and the infant is fussy and hungry after vomiting.
- If undiagnosed, dehydration, metabolic alkalosis, and failure to thrive may occur.
- Precise etiology is unknown, but HPS is more common in boys by four to six times than in girls. It is also less common in African-American infants than Caucasian infants, and rare in Asians. Inheritance is polygenic, with an increased risk in the siblings and offspring of affected persons.
Pathophysiology
The circular muscle of the pylorus thickens as a result of hypertrophy. This produces severe narrowing of the pyloric canal between the stomach and the duodenum. Consequently, the lumen at this point is partially obstructed. Over time the size of the opening is reduced, and the partial obstruction may progress to complete obstruction.
Clinical Manifestations
The infant will begin vomiting as early as 1 week and as late as 5 months, usually at 3 weeks of age. Vomiting episodes normally occur immediately after each feeding.
- Nonbilious vomiting, as the vomitus originates from the stomach, not reaching the duodenum where bile is deposited. Vomitus may become brown or blood-tinged if gastritis develops.
- Projectile vomiting may occur and appear progressively. Vomitus may reach as far as 3 to 4 feet if side-lying and 1 feet if back-lying.
- Prolonged vomiting may lead to dehydration, weight loss, and failure to thrive.
- Gastric peristalsis (left-to-right) may become visible during examination. The upper abdomen may also be visible distended.
- An olive-shaped mass in the epigastrium, just to the right of the umbilicus may be palpated.
- The infant may display hunger; avid feeding even after vomiting. Other than chronic hunger, no pain or discomfort may be noted.
Diagnostic Evaluation
A diagnosis is often made after the history and physical examination.
- The olive-like mass is most easily palpated when the stomach is empty, the infant is quiet, and the abdominal muscles are relaxed.
- Ultrasonography can demonstrate an elongated mass surrounding a long pyloric canal. If this is not observed, GI radiography should be done to rule out other causes of vomiting.
- Laboratory findings can display fluid and electrolyte imbalances if the condition is not diagnosed early.
- Lowered sodium and potassium levels are present, but may be masked by proportional hemoconcentration.
- A greater diagnostic value is placed on chloride levels and a corresponding rise in pH and bicarbonate, indicative of metabolic alkalosis.
Management
The standard therapy instituted is a pyloromyotomy (pyloroplasty). Preoperatively, infants with evidence of fluid and electrolyte imbalances must be rehydrated and metabolic alkalosis must be corrected via parenteral fluid and electrolyte administration. This may delay surgery by 24 to 48 hours. NG tube decompression may be required for infants who continue to vomit.
A pyloromyotomy or the Fredet-Ramstedt operative procedure is a high-success procedure often performed via laparoscope that involves the creation of a longitudinal incision through the circular muscle fibers of the pylorus down to, but not including, the submucosa (refer to Figure B in the image above)
Postoperatively, feedings may be continued within 4 to 6 hours, beginning with small, frequent feedings of water or electrolyte solutions. If these are retained, about 24 hours after surgery formula is started in the same small increments. The amount and the interval between feedings is gradually increased until a full feeding schedule is reinstated, which usually takes about 48 hours.
The nurse primarily observes for clinical features that help establish the diagnosis, careful regulation of fluid therapy, and reestablishment of normal feeding patterns.
- HPS should be considered a possibility in infants who fail to gain weight and has a history of vomiting after feedings. Assessment should be based on observation of eating behaviors, evidence of characteristic clinical manifestations, hydration, and nutritional status.
- Preoperatively, NPO is begun and IV of dextrose, sodium chloride, and added potassium may be indicated. The nurse should assess skin and mucous membrane status for alterations in hydration status.
- Infants who are receiving IV fluids may be given a pacifier to meet nonnutritive sucking needs.
- Stomach decompression and gastric lavage may be done. The nurse is responsible for ensuring NG patency, functioning, and documentation of drainage.
Provide support for the patients. Involve them in the care of the infant when necessary and reassure them that the condition was the result of a structural problem and that it is not a reflection of their parenting skills and capacities.
Feeding is instituted within several hours postoperatively, beginning with clear liquids. They are offered in small quantities at frequent intervals. If the infant has been breastfed, breast milk expressed by the mother may be given by bottle when the infant is able to tolerate feedings, or the mother is instructed to limit nursing time and gradually increase the time to previous patterns. Supervision of feedings is an important part of postoperative care.
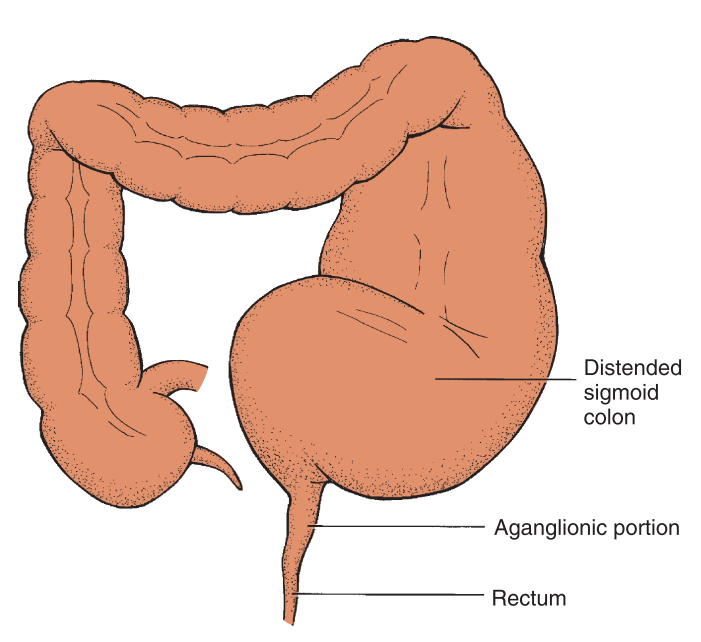
Aganglionic Megacolon
Hirschsprung’s disease (HD) is a congenital anomaly that results in mechanical obstruction from inadequate motility of part of the intestine. Its etiology is unknown, but it is more common in males than females.
Pathophysiology
Aganglionosis of the intestine results in a loss of the rectosphincteric reflex and an abnormal microenvironment of the cells of the affected intestine. The term congenital aganglionic megacolon describes the primary defect, which is the absence of ganglion cells. The reduction of enteric nervous system stimulation inhibits the internal sphincter’s ability to relax. Because ganglion cells are parasympathetic, sympathetic stimulation of the intestine remains unopposed, resulting in increased intestinal tone.
Clinical Manifestations
- Failure to pass meconium within 24 to 48 hours
- Bilious vomiting
- Abdominal distention
- Constipation
- Ribbonlike, foul-smelling stools
- Visible peristalsis
- Refusal to feed
- Easily palpable fecal mass
- Failure to thrive; Undernourished, anemic appearance
Diagnostic Evaluation
In neonates, the diagnosis is initially suspected on the basis of clinical signs of intestinal obstruction or failure to pass meconium. In infants and children the history is an important part of diagnosis and typically includes a chronic pattern of constipation.
- Rectal Examination: absence of feces and tightness of internal sphincter. Leakage of liquid stool and accumulated gas may occur upon examination if the affected segment is short.
- Contrast Enema: visualization of the transition point between the aganglionic distal segment and the dilated proximal colon (megacolon). However, this may only become evident in children two months of age or older.
- Rectal Biopsy: a biopsy is confirmatory once it determines the absence of ganglion cells from a full-thickness or suction biopsy.
- Rectal Manometry: a balloon catheter is inflated in the rectum to apply pressure to the rectal wall and attempt to stimulate the internal anal sphincter. It measures pressure applied by the internal and external sphincter in response to the balloon. A normal finding will show a relaxation of the internal sphincter followed by a contraction of the external sphincter. In HD the external sphincter contracts normally but the internal sphincter fails to relax.
Management
Most children with HD require one of three operative procedures once the child is stabilized with fluid and electrolyte replacement and colonic cleansing (enemas).
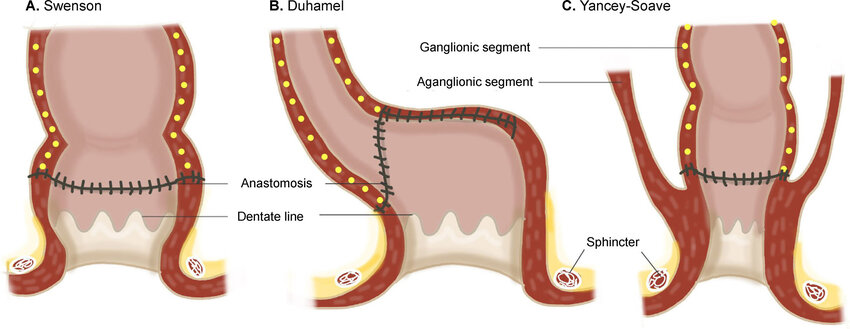
- Soave pull-through procedure (most common)
- Swenson procedure
- Duhamel procedure
Nursing care will depend on the age of the child and type of treatment being used.
- Neonate: the primary focus is to aid the parents adjust to a congenital defect in their child, foster infant-parent bonding, prepare the parents for medical-surgical intervention, and prepare the parents to assume the care of the child after surgery.
- Monitoring for complications: the most serious complication of HD is enterocolitis. Preoperative care may include decreasing bacterial flora with oral or systemic antibiotics and colonic irrigations using antibiotic solution. In neonates, this may not be necessary as the bowels are still sterile.
- Postoperative Care: involve and aid the parents of the child in caring for the child. Allow them to help with feedings and observe for signs of wound infection, irregular passage of stool (constipation or true incontinence), or the development of complications.
- Measure abdominal girth daily and as necessary.
- Assess the surgical site for redness, swelling, and drainage.
- Assess the stoma (if a colostomy was done) for bleeding or skin breakdown. The stoma should be pink-red and moist.
- Maintain NPO status until bowel sounds return or flatus is passed, usually within 48 to 72 hours.
- Maintain the nasogastric tube to allow intermittent suction until peristalsis returns.
- Maintain IV fluids until the child tolerates appropriate oral intake, advancing the diet from clear liquids to regular as tolerated and as prescribed.
- Preventing Complications: anal strictures are a potential problem after surgery. Daily dilatations may be required, which can be done by parents who can be taught to perform care at home.
- Colostomy Care: a diverting colostomy may be used in some cases of HD. Parents are taught about the use and care of colostomy appliances